Headache Treatment
Headache types and causes

Headaches can come in a wide variety of types, with different symptoms, causes and severity. Some headaches can be particularly debilitating, such as cluster headaches or migraines. Some headaches may have a a soft tissue component, which include ligaments, tendons, muscles, bursae fascia and parts of joint structures. Changes to such tissues can impact joint mechanics, stability and tensional forces leading to pain. Hydration levels, diet (vitamins and minerals) and even medications can play a significant part in some cases. Headaches can also occur due to specific medical conditions with varying levels of seriousness. Any sudden and out of the ordinary severe headaches (the worst headache ever) can require prompt medical attention and investigation. Fortunately, and as common as headaches are, cases of serious medical emergencies are less common. Some of the more common headaches include:-
- Tension
- Cluster
- Cervicogenic
- Migraines
- Sinus (allergies, inflammation)
- Hormonal (changes in bodily cycles)
- Medications or stimulants related (too much, or withdrawal)
Headache treatments

The drug market for migraine treatments alone is a multi-billion dollar industry, just a fraction of the overall headache market. Many of the routinely taken over the counter headache medications have side effects. Research shows the adverse longer-term impacts of continued use of many common headache drugs. Also, some drug companies have found themselves in hot water due to product marketing. Claims of faster-acting products or being made for migraines were common in such cases. However, the products contained the same generic active ingredients yet different packaging and premium prices.
Attempting to mask symptoms or pain is not the best strategy. Addressing the reason for symptoms and stopping things from gradually getting worse makes more sense. In some, cases headaches may require medications to treat the underlying cause, though such drugs may need a doctor's prescription. Equally, eye strain can create headaches and might be a sign of needing glasses and a visit to an Optometrist. However, many types of headaches have muscular or myofascial origin.
Prevention and habits

Fortunately, it is possible to resolve or reduce the frequency of the vast majority of headaches with some simple lifestyle changes and education about contributory factors. Many headaches can have a muscular or fascial component, resulting in musculoskeletal tension. Our habits or how we use our bodies can play a huge part in how bodily tissues react to what is demanded of them. Habits can include sleeping position, type of work, hydration levels, general physical activity levels, diet, work setup, frequency of breaks, hobbies, interests, previous injuries, etc. Many professions involve a lot of computer work, either within an office environment or remotely. An ergonomic computer setup is relatively easy to achieve for little cost, yet it can hugely impact tissue loading and pain. Equally, our sleeping position and a correctly supported head and neck can also make a massive difference in tissue loading. Hence, pillow height and support can be relevant to headaches, migraines, and neck, shoulder, and back pain. Any combination of these factors can result in muscular tension and myofascial trigger points(MTrP's). There are many muscles in the back, neck, shoulders and head, which can directly or indirectly refer to pain. Notably, the imaging has shown the presence of myofascial trigger points in people suffering from some types of headaches, including migraines (Sollmann et al., 2019; Heldarskard et al., 2018).
Muscular Tension and Stress

It is relatively easy to see and feel the impact of muscle tension on headache onset. Working on a sofa with a laptop on the lap will soon create tension in the shoulders, neck and back muscles. Grinding one's teeth affects muscles of the jaw and head. Equally, walking in the mountains in the cold and wind tenses the muscles of the forehead and face. Any of the activities just covered may lead to a headache, with slightly different pain patterns, symptoms and severity.
Another factor that can play a significant part in headache onset is stress, which has Physiological and Psychological aspects (see the related articles on stress regarding "stressors"). Stress or "stressors" can come in many forms, physical, emotional, psychological, environmental etc. Besides stress causing muscle tension (armouring), it can also affect other bodily systems, including various hormone levels. The effects of stress can add a wide variety of contributory factors to the formation of headaches, severity and even symptoms. Stress can affect everything from the type of foods we crave to sleep patterns, and lack of sleep can impact our perception of pain. Stress is a widespread factor with migraine headaches, and some research shows that myofascial trigger points(MTrPs) can play a part. The presence of myofascial trigger points in the neck and shoulders of students with depression, anxiety and stress has also been noted (Kashif et al., 2021).
Myofascial Trigger Points (MTrPs) and pain
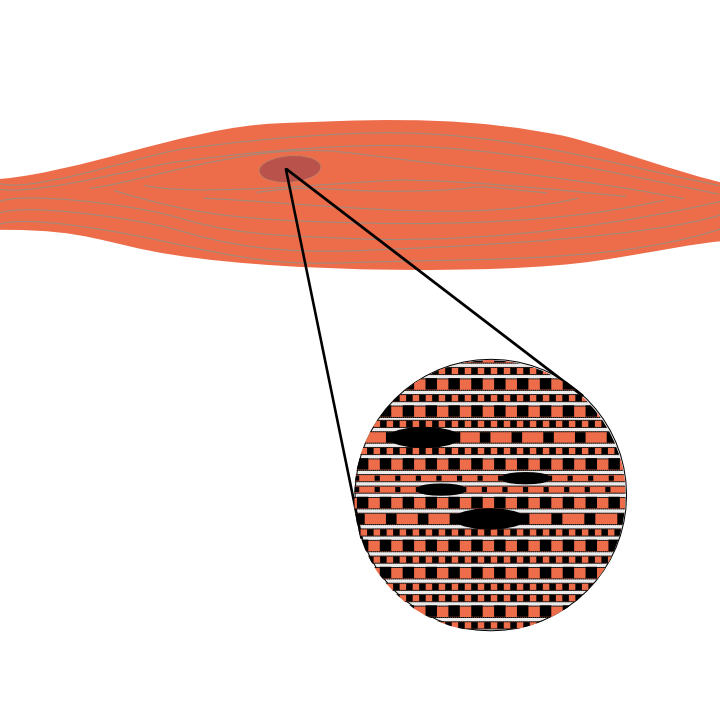
Trigger points (TrPs) are taut bands of hyperirritable soft tissue and are known as active or latent. Active trigger points are typically painful to touch, can cause pain referral, and often hurt when moving. Latent trigger points tend not to produce pain when pressed or during movement. Either type of TrP would still affect Biotensegrity and Tissue Adaptation (see related articles). Latent trigger points may become Active at some stage and vice versa. Both trigger points are palpable, though different from a muscle spasm. A muscle spasm involves a painful involuntary contraction of all fibres within a muscle, bringing the origin and insertion ends of the muscle closer together. Spasms also tend to involve a type of pulsation or contractions and sometimes a tearing sensation, all of which can prove extremely painful. The taut bands within trigger points are small sections of muscles fibres, which have become stuck in a contracted state. Although trigger points may produce a deep throbbing type of pain, they do not have a spasm's severe and repeated pulsating contractions.
The very existence of myofascial trigger points has a somewhat controversial history. The general medical profession has historically used the term pseudoscience for such things. Manual therapists have known about trigger points, though under differing terms since the origins of manual therapy. Equally, many manual therapists and bodyworkers are aware of the links between TrP's and many types of headaches, including migraines due to palpation. Although the telltale signs of trigger points are palpable (one can feel them), historically, TrP's were not visible on imaging, such as x-rays, CT scans, MRI or ultrasound. However, the presence or absence of pathology on imaging can relate to limitations of the technology and does not always indicate relevance (see the article on back pain and disc pathologies). More recent research and advances in MRI T2-weighted imaging have shown the presence of trigger points in the upper trapezius muscle of migraine sufferers. Equally, myofascial pain associated with neck and shoulder trigger points appears to be a component of other types of headaches and migraines.
Muscle Tension, Treatment and Prevention
The author has historically suffered from migraines himself and treated other migraine sufferers for over 16 years and so is well aware of contributory factors. Based on the author's clinical experience, key factors include hydration levels, "stressors", and myofascial trigger points, even if specific research is limited. Often, treatment and prevention involve a combination of strategies to treat the symptoms and cause(s). Such a process requires effort from both the patient and therapist. A good therapist can help educate the patient on causal factors and prevention strategies. Equally, soft tissue treatment can provide symptom relief in many cases of headache pain. However, treatment alone tends to treat the symptoms, hence the importance of following prevention advice. Chronic cases can require more work on the therapist and certainly the patient. Typically, the passage of time in the case of Persistent Pain conditions leads to many soft tissue adaptations (see the related articles section). This situation means more work is required to get tissues back to functioning normally again, and one area affects another (see the kinetic chain for a simple explanation or the Biotensegrity related article for more in depth view).
Many manual therapy techniques can effectively treat many types of headaches, especially when combined with patient education. Many myofascial release (MFR) techniques can effectively treat trigger point pain. Some methods, such as dry needling (DN) or neuromuscular therapy (NMT), aim to treat trigger points. Other techniques, such as Gua Sha, do not specifically target trigger points but can be very effective with some types of headaches. Methods including positional release technique (PRT) and soft tissue release (STR) can also prove effective when dealing with trigger points and even muscle spasms.
Myofascial Pain Relief - Treatment and Techniques
- Dry Needling - DN
- Soft Tissue Release - STR
- IASTM - Instrument-Assisted Soft Tissue Mobilisation
- Gua Sha treatment
- Muscle Energy Technique - MET
- Neuromuscular Therapy - NMT
- Positional Release Technique - PRT
The article was written by Terry Davis MChiro, GradCertMentHlth, BSc. (Hons), Adv. Dip. Rem. Massag., Cert. WHS.
If you liked this article or found it interesting, feel free to share the content with others. There are lots more articles available via the TotalMSK main Health, Wellness and Sports Injury blog page, which has a brief description of all the articles to date.
About the Author
As of December 31st 2020, the author chose to leave the Chiropractic profession due to a planned move back to Australia, where his training and education are not recognised. Terry no longer works as a Chiropractor and works as a Myotherapist in Morningside, Brisbane. He developed an early interest in soft tissue therapy and Myofascial Release Techniques and that interest has continued to develop since 2006. Terry's interests in human performance and trauma have naturally led to him developing a specialism in treating work and sports-related musculoskeletal injuries and Chronic Pain symptoms.
The author possesses an unusual background for somebody who trained in the McTimoney Chiropractic technique. His education, training, and practical experience span over two decades and relate to health's physical and mental aspects. He also needed to push his body and mind to the limits of physical and psychological endurance as part of his time serving in Britain's elite military forces. His education includes a bachelor of science degree in Business Management, with a specialisation in psychology and mental health in the workplace, an Masters of Chiropractic, MChiro, a Postgraduate Certificate in Mental Health and a multitude of soft tissue therapy qualifications (see the about section for more details). His soft tissue qualifications range from certificate level right through to a BTEC Level 5 Advanced Diploma in Clinical Sports and Remedial Massage Therapy. He has also taught as a senior course coach teaching Remedial Massage and the Advanced Diploma Myotherapy in Australia. His teaching involved both theoretical and practical aspects, including advanced Myofascial Release Techniques and has certification in training and assessment. Terry will have taught many of the first students to train as Myotherapists in Brisbane. Terry's combination of knowledge through education, training, elite military service, and personal injury history has paid dividends for the patients he sees and has treated over the last 19 years. Terry is still extremely active and enjoys distance running, kayaking, mountain biking and endurance-type activities.